Pediatric Pulmonologist Near Me: Unlocking Expert Care for Children’s Respiratory Issues. As a parent, there’s no greater fear than seeing your child struggle to breathe. When symptoms persist, it’s essential to find a trusted pediatric pulmonologist who offers expert care for your child’s respiratory issues.
A pediatric pulmonologist specializes in diagnosing and managing respiratory problems in infants, children, and adolescents. With advanced training and expertise, they address a wide range of respiratory conditions, from mild asthma to severe lung diseases.
Definition of a Pediatric Pulmonologist and Their Role in Treating Respiratory Issues

A Pediatric Pulmonologist is a medical specialist who dedicates their expertise to diagnosing and managing respiratory problems in infants, children, and adolescents. These specialists often work closely with pediatricians and other healthcare professionals to ensure that young patients receive the best possible care for a wide range of respiratory conditions.
Qualifications and Training
To become a pediatric pulmonologist, one typically needs to complete a residency program in pediatrics after earning a medical degree (MD) or a Doctor of Osteopathic Medicine (DO) degree. After the residency, they must pursue additional specialized training in pediatric pulmonology through a fellowship program. This specialized training program usually lasts one or two years and provides hands-on experience in diagnosing and treating respiratory problems in children.
Unique Qualifications
Pediatric pulmonologists must possess a unique combination of knowledge, skills, and traits that set them apart from other medical specialists. They must be able to understand the complexities of pediatric respiratory health, including the anatomical, physiological, and psychological aspects of childhood and adolescent development. They must also be skilled in a wide range of diagnostic and therapeutic techniques, including advanced imaging and respiratory monitoring. Additionally, they must have strong communication skills to effectively interact with pediatric patients, their families, and other healthcare professionals.
Medical Institutions and Settings
Pediatric pulmonologists can be found working in various medical institutions and settings, including:
* Children’s hospitals
* Pediatric clinics
* Academic medical centers
* Community hospitals with pediatric departments
* Private practice clinics
Most Common Respiratory Conditions Treated, Pediatric pulmonologist near me
Some of the most common respiratory conditions treated by pediatric pulmonologists include:
- Asthma: A chronic condition characterized by inflammation and constriction of the airways, leading to wheezing, coughing, and shortness of breath.
- Cystic Fibrosis: A genetic disorder that affects the respiratory, digestive, and reproductive systems, causing thick, sticky mucus to build up in the lungs and digestive tract.
- Chronic Lung Disease: A group of conditions that can cause scarring and inflammation in the lungs, leading to breathing difficulties and other complications.
- Respiratory Infections: Bacterial, viral, or fungal infections that can cause inflammation and damage to the respiratory system, leading to symptoms such as coughing, fever, and difficulty breathing.
Advanced Diagnostic Tools and Procedures Used by Pediatric Pulmonologists to Identify Respiratory Conditions
Pediatric pulmonologists use a range of advanced diagnostic tools and procedures to evaluate respiratory problems in children. These tools help identify underlying conditions, monitor disease progression, and inform treatment decisions. With the latest technology and techniques, pediatric pulmonologists can accurately diagnose and manage respiratory conditions in children.
Imaging Studies: Chest X-rays and Computed Tomography (CT) Scans
Imaging studies are a crucial component of respiratory diagnosis. Pediatric pulmonologists use chest X-rays and CT scans to visualize the lungs and airways, identifying abnormalities such as pneumonia, bronchiolitis, and asthma exacerbations. Chest X-rays provide a quick and simple way to diagnose common respiratory conditions, while CT scans offer a more detailed view of the lungs, helping to diagnose conditions like bronchiectasis and cystic fibrosis.
- Chest X-rays are commonly used to diagnose pneumonia, bronchiolitis, and asthma exacerbations.
- CT scans are used to diagnose more complex conditions, such as bronchiectasis, cystic fibrosis, and lung cancer.
- Imaging studies can also help monitor disease progression and response to treatment.
Bronchoscopy and Laryngoscopy Procedures
Bronchoscopy and laryngoscopy are procedures used to visualize the airways and diagnose respiratory conditions. During a bronchoscopy, a flexible tube with a camera is inserted through the nose or mouth and guided down the airway, allowing the pediatric pulmonologist to examine the lungs and airways for abnormalities. Laryngoscopy involves the insertion of a scope through the mouth to examine the vocal cords and larynx.
- Bronchoscopy helps diagnose conditions like asthma, chronic cough, and lung cancer.
- Laryngoscopy is used to diagnose conditions like vocal cord paralysis and laryngitis.
- Both procedures can also be used to remove foreign bodies and secretions from the airways.
Other Diagnostic Tools and Procedures
Pediatric pulmonologists may also use additional diagnostic tools and procedures, such as pulmonary function tests (PFTs), sleep studies, and arterial blood gas (ABG) tests, to evaluate respiratory function and diagnose underlying conditions.
- PFTs help measure lung function and capacity.
- Sleep studies help diagnose sleep apnea and other sleep-related breathing disorders.
- ABG tests measure oxygen and carbon dioxide levels in the blood.
Creating a Pediatric Pulmonologist’s Treatment Plan for Respiratory Conditions – A Step-by-Step Guide: Pediatric Pulmonologist Near Me
A pediatric pulmonologist’s primary goal when treating respiratory conditions in children is to develop a comprehensive treatment plan that addresses the unique needs of each child and their family. This plan involves a multidisciplinary approach, often involving input from specialists such as pediatric surgeons, radiologists, and geneticists. By understanding the specific needs of each child, pediatric pulmonologists can create tailored treatment plans that maximize the chances of successful outcomes.
Step 1: Initial Consultation and Diagnosis
During the initial consultation, the pediatric pulmonologist conducts a thorough medical examination, reviewing the child’s medical history and gathering information from the child’s family members. This helps to identify the underlying cause of the respiratory condition. The doctor may also perform diagnostic tests such as chest X-rays, blood tests, or pulmonary function tests to confirm the diagnosis. In some cases, the pediatric pulmonologist may order additional tests such as bronchoscopy or endoscopy to gather more information.
Step 2: Developing a Personalized Treatment Plan
Based on the diagnosis and test results, the pediatric pulmonologist works with the child’s family to develop a personalized treatment plan. This plan takes into account the child’s age, medical history, and overall health. The treatment plan may include medication, lifestyle modifications, and other interventions to manage the respiratory condition. The pediatric pulmonologist also educates the family on how to use the medication, monitor the child’s condition, and make any necessary adjustments to the treatment plan.
Step 3: Managing Symptoms and Complications
The pediatric pulmonologist plays a crucial role in managing symptoms and complications associated with the respiratory condition. This may involve prescribing medication to alleviate symptoms such as coughing, wheezing, or shortness of breath. The doctor may also recommend lifestyle modifications such as avoiding allergens, quitting smoking, or increasing physical activity. In some cases, the pediatric pulmonologist may need to manage complications such as pneumonia, bronchiolitis, or asthma exacerbations.
Step 4: Monitoring Progress and Adjusting the Treatment Plan
Regular follow-up appointments with the pediatric pulmonologist are essential to monitor the child’s progress and adjust the treatment plan as needed. The doctor may use various tools such as pulmonary function tests, chest X-rays, or blood tests to track the child’s condition. Based on the test results, the pediatric pulmonologist may need to adjust the treatment plan, introduce new medications, or make lifestyle changes to improve the child’s outcomes.
Step 5: Coordination with Other Healthcare Providers
In some cases, the pediatric pulmonologist may need to coordinate care with other healthcare providers such as pediatricians, surgeons, or anesthesiologists. This may involve working with a multidisciplinary team to develop a comprehensive treatment plan that addresses the child’s overall health needs. The pediatric pulmonologist may also refer the child to specialists such as allergists, immunologists, or geneticists for further evaluation and care.
Step 6: Ongoing Education and Support
The pediatric pulmonologist plays a vital role in educating the child’s family on how to manage the respiratory condition and prevent complications. The doctor may provide information on medication use, lifestyle modifications, and how to recognize signs of worsening symptoms. The pediatric pulmonologist may also offer ongoing support and guidance to help the family navigate the healthcare system and make informed decisions about the child’s care.
Building a Support Network for Children with Respiratory Conditions – Collaboration Between Pediatric Pulmonologists and Other Healthcare Providers
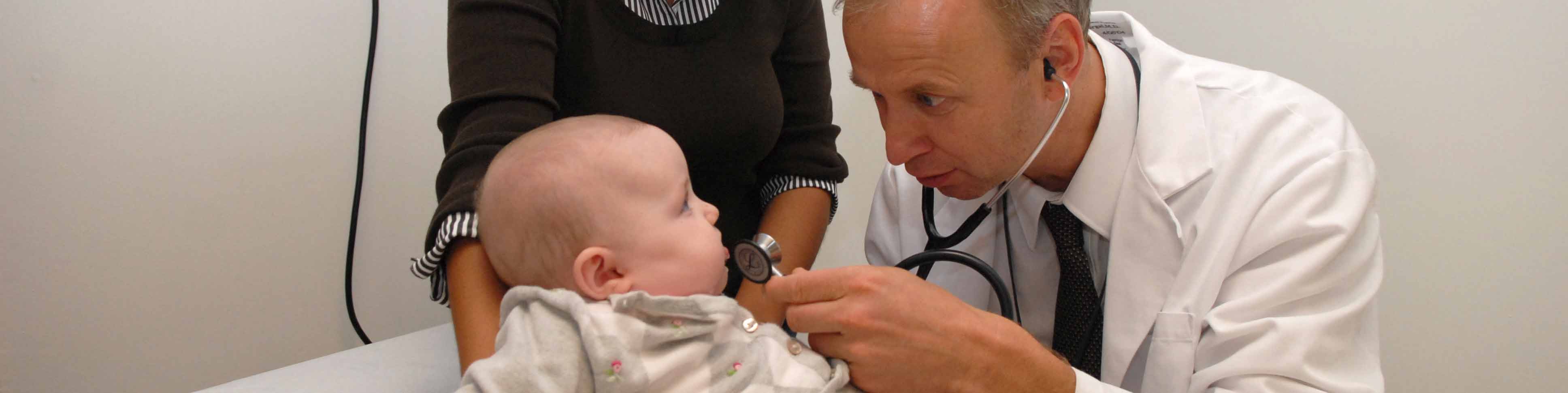
In Surabaya, Indonesia, kids with respiratory conditions often require a team of healthcare providers to manage their care. Pediatric pulmonologists play a crucial role in coordinating this care to ensure that kids receive the best possible treatment. By working together with other healthcare providers, pediatric pulmonologists can provide comprehensive care to kids with respiratory issues.
Referrals to Specialists and Hospitals
When kids need specialized care or hospitalization, pediatric pulmonologists collaborate with other healthcare providers to arrange referrals. These referrals might be to pediatric intensivists for children who require intensive care, or to surgical specialists for children who need lung surgery. This streamlined process ensures that kids receive the most appropriate care in the right setting.
- Pediatric pulmonologists work closely with pediatric intensivists to ensure that kids receive the best possible care in the intensive care unit (ICU).
- They also collaborate with surgical specialists to arrange for complex lung surgeries, such as lung transplants or pneumonectomies.
- Futhermore, pediatric pulmonologists may refer kids to cardiologists for children who have heart conditions that affect their breathing.
Collaboration with Pediatricians and Specialists
Pediatric pulmonologists often work with pediatricians to manage kids’ care in the outpatient setting. They may also collaborate with other specialists, such as allergists or gastroenterologists, to ensure that kids receive comprehensive care. For example, a pediatric pulmonologist might work with a pediatrician to develop a treatment plan for a child with asthma, while also consulting with an allergist to identify and avoid triggers.
- Pediatric pulmonologists work with pediatricians to develop treatment plans for kids with asthma, chronic cough, or other respiratory conditions.
- They also collaborate with specialists, such as allergists, to identify and treat underlying conditions that may be contributing to kids’ respiratory symptoms.
- Pediatric pulmonologists may work with gastroenterologists to manage kids with reflux disease or other conditions that affect their breathing.
Benefits of Collaboration
The collaboration between pediatric pulmonologists and other healthcare providers has numerous benefits for kids with respiratory conditions. By working together, healthcare providers can ensure that kids receive comprehensive, coordinated care. This approach has been shown to improve outcomes for kids, reduce lengths of stay, and decrease hospital readmissions.
- Collaboration between pediatric pulmonologists and other healthcare providers has been shown to improve outcomes for kids with respiratory conditions.
- This approach reduces lengths of stay and decreases hospital readmissions.
- Collaboration also ensures that kids receive comprehensive, coordinated care that addresses all aspects of their condition.
Wrap-Up
Don’t let respiratory issues hold your child back. By finding a pediatric pulmonologist near you and taking advantage of their care, you can empower your child to live a healthy, happy life. With the right medical guidance, you can navigate even the most challenging respiratory concerns and ensure the best possible outcomes for your family.
FAQ
Q: What services do pediatric pulmonologists offer to treat children’s respiratory issues?
Pediatric pulmonologists offer a range of diagnostic, management, and therapeutic services, including spirometry, airway clearance techniques, and bronchoscopies.
Q: How do I find a pediatric pulmonologist near me?
You can start by searching online, checking with your pediatrician for referrals, or contacting local hospitals and medical institutions for recommendations.
Q: What are the signs that my child needs to see a pediatric pulmonologist?
Signs that your child may need a pediatric pulmonologist’s care include persistent coughing, wheezing, difficulty breathing, or recurring respiratory infections.
Q: How often should my child visit a pediatric pulmonologist?
The frequency of visits depends on your child’s specific respiratory condition and needs, but regular check-ups and monitoring are crucial for optimal care.