iud removal near me sets the stage for this enthralling narrative, offering readers a glimpse into a story that is rich in detail and brimming with originality from the outset.
This guide is a comprehensive resource for women seeking to understand the process of IUD removal, from the initial decision to remove the device to the post-procedure recovery and potential long-term effects on fertility and reproductive health.
Choosing the Right Time for IUD Removal
When considering removal of a intrauterine device (IUD), it’s essential to choose the right time to ensure a safe and successful procedure. The ideal time frame for IUD removal varies depending on several factors, including age, fertility goals, and menstrual health.
The American College of Obstetricians and Gynecologists (ACOG) recommends removing an IUD between 4-10 years after insertion, with the average removal time ranging from 5-7 years. However, this timeframe may need to be adjusted based on individual circumstances.
Factoring in Age and Fertility Goals
If you’re under 40 and still hoping to conceive, it’s recommended to remove the IUD at the recommended timeframe or earlier. This is because fertility declines with age, and delaying removal may reduce the chances of conception.
For women over 40, the decision to remove the IUD may be based on more personal and health-related factors, such as menopausal transition or concerns about hormone-related symptoms.
Considering Menstrual Health
If you experience persistent pelvic pain, heavy bleeding, or other menstrual irregularities after IUD insertion, removal should be considered. These symptoms may be signs of complications or the body’s reaction to the device.
Preparation for IUD Removal
Before the procedure, your healthcare provider may recommend several tests, including:
A pelvic exam to assess the condition of your cervix and uterus.
Ultrasound to determine the IUD’s position and ensure it hasn’t perforated the uterus.
A blood test to check for any underlying infections or disorders.
Your healthcare provider may also prescribe medications to help manage any bleeding or discomfort during and after the procedure.
Potential Signs and Symptoms Indicating IUD Removal
If you experience any of the following symptoms, it’s essential to consult your healthcare provider for removal:
Persistent pelvic pain or discomfort.
Heavy bleeding or prolonged menstrual periods.
Increased menstrual cramps or spotting.
Feeling of the IUD moving or protruding from the cervix.
Preparing for IUD Removal
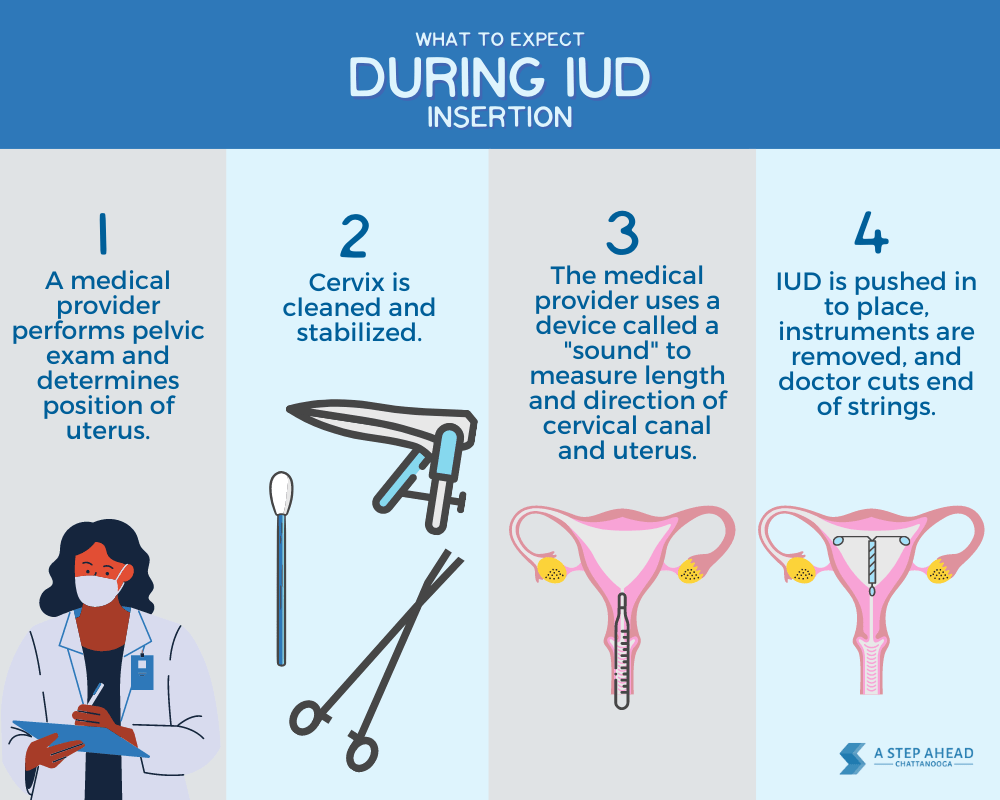
Preparing for IUD removal involves several physical and emotional considerations to ensure a smooth and successful procedure. It’s essential to take the necessary steps before the procedure to minimize potential risks and complications.
Step-by-Step Checklist for IUD Removal Preparation
To prepare for IUD removal, follow these steps:
-
Schedule a pre-procedure appointment with your healthcare provider to discuss any concerns or questions you may have.
This appointment will also give your healthcare provider an opportunity to review your medical history and ensure you are a good candidate for IUD removal. -
Stop using birth control at least 14 days before the procedure if you’re using hormonal forms of birth control.
This will help regulate your menstrual cycle and reduce the risk of complications. -
Discuss your menstrual cycle and any concerns you may have with your healthcare provider.
They may recommend taking pain medication or other measures to manage discomfort during and after the procedure. -
Consider speaking with a therapist or counselor about any emotional concerns you may have regarding IUD removal.
This can help you process your feelings and develop a support network for after the procedure. -
Arrange for someone to drive you home after the procedure and provide support for several hours.
This ensures you have proper recovery support and can focus on rest and relaxation.
Menstrual Management Before IUD Removal
During the days leading up to the procedure, it’s essential to manage your menstrual cycle to ensure your healthcare provider can perform the removal effectively and safely. You may need to:
-
Stop using birth control to help regulate your menstrual cycle.
This can help your healthcare provider identify any potential issues, such as heavy bleeding or spotting, that may affect the procedure. -
Take pain medication as directed by your healthcare provider.
This will help manage any cramping or discomfort you may experience during and after the procedure. -
Pack a small bag with essentials like underwear, snacks, and a change of clothes.
This will come in handy during and after the procedure, especially if you need to stay overnight in the hospital or clinic.
Pain Control and Recovery
While IUD removal is generally a quick and relatively easy procedure, some women may experience discomfort or pain during or after the procedure. Your healthcare provider will discuss pain management options with you beforehand, and you may need to:
-
Take pain medication as directed to help manage cramping and discomfort.
Your healthcare provider may recommend a specific type of pain medication, such as ibuprofen or acetaminophen, to help minimize pain. -
Use a heating or cooling pad to help alleviate cramps and discomfort.
Applying heat or cold to the abdomen can help reduce cramping and promote relaxation. -
Rest and relax for several hours after the procedure.
Your body needs time to recover from the procedure, and getting plenty of rest will help your uterus return to its normal state.
Potential Complications and Emergencies During IUD Removal
While IUD removal is generally a safe procedure, there are potential complications and emergencies that may arise. Your healthcare provider will discuss these risks with you beforehand, but some possible complications and their emergency response protocols include:
-
Heavy bleeding or spotting.
If you experience heavy bleeding or spotting, your healthcare provider may administer medication to help stop the bleeding or insert a special device to help control it. -
Cramping or pain.
If you experience severe cramping or pain, your healthcare provider may administer pain medication or recommend other measures to alleviate discomfort. -
Infection.
If you experience signs of infection, such as fever or redness, your healthcare provider may prescribe antibiotics to help clear the infection. -
Uterine perforation.
This is a rare but serious complication where the IUD is inserted into the uterine wall or other surrounding tissue. Your healthcare provider may need to perform emergency surgery to remove the IUD and repair any damage.
Choosing a Qualified Healthcare Provider for IUD Removal
When it comes to IUD removal, finding the right healthcare provider is crucial for a safe and successful procedure. With various types of healthcare professionals available, it can be overwhelming to decide who to trust with this important decision. In this article, we will explore the different types of healthcare providers who can perform IUD removal, share stories of women who have successfully found healthcare providers, and provide a comparison of costs and insurance coverage options for IUD removal services.
Types of Healthcare Providers for IUD Removal
Several types of healthcare providers can perform IUD removal, each with their own qualifications and expertise. Obstetricians, gynecologists, and nurse practitioners are among the most common healthcare providers for IUD removal.
Obstetricians
Obstetricians specialize in pregnancy, childbirth, and women’s reproductive health. They are trained to perform IUD removal procedures and can provide guidance on reproductive health. Obstetricians often have a wide range of expertise and can provide comprehensive care for women’s health.
Gynecologists
Gynecologists specialize in women’s reproductive health and the diagnosis and treatment of disorders related to the female reproductive system. They are trained to perform IUD removal procedures and can provide guidance on reproductive health. Gynecologists often have specialized knowledge and can provide expert care for women’s health.
Nurse Practitioners
Nurse practitioners are advanced practice registered nurses who have specialized training in primary and specialty care. They are qualified to perform IUD removal procedures and can provide guidance on reproductive health. Nurse practitioners often have strong relationships with their patients and can provide personalized care.
Real-Life Stories: Finding Healthcare Providers for IUD Removal
Here are a few stories of women who have successfully found healthcare providers for IUD removal:
* “I was nervous about finding a healthcare provider for IUD removal, but my primary care physician referred me to a gynecologist who specialized in IUD removal. She was kind, professional, and made me feel at ease throughout the entire process.” – Emily
* “I was lucky to have a nurse practitioner as my healthcare provider. She was knowledgeable, compassionate, and made sure I had all the information I needed to make informed decisions about my reproductive health.” – Sophia
* “I had a great experience with my obstetrician. She was attentive, answered all my questions, and made sure I was comfortable throughout the procedure.” – Rachel
Costs and Insurance Coverage for IUD Removal Services
The cost of IUD removal services can vary depending on the healthcare provider, location, and insurance coverage. Here is a comparison of costs and insurance coverage options for IUD removal services at various healthcare providers:
| Healthcare Provider | Cost Range | Insurance Coverage |
| — | — | — |
| Obstetricians | $500-$1,500 | Private insurance, Medicare, Medicaid |
| Gynecologists | $600-$2,000 | Private insurance, Medicare, Medicaid |
| Nurse Practitioners | $400-$1,200 | Private insurance, Medicare, Medicaid |
Note: Costs may vary depending on the location and healthcare provider.
IUD Removal Aftercare: Managing Side Effects and Recovering Fast

IUD removal aftercare is a crucial aspect of the overall process, focusing on managing side effects and aiding recovery. Proper care and attention during this period will help minimize complications and ensure a smooth transition.
The typical recovery time frame for IUD removal can vary depending on individual circumstances, but most women can return to their normal activities within a few days to a week. It’s essential to follow the provided guidelines by your healthcare provider for post-procedure care.
Managing Common Side Effects
Cramping, bleeding, and emotional distress are common side effects experienced by some women after IUD removal. These symptoms can be managed effectively with the right approach:
- Over-the-counter pain relief medication, such as ibuprofen or acetaminophen, can help alleviate cramping and discomfort.
- Bleeding may be heavier than menstrual periods, but it should stop within a few days to a week. Monitor your flow and report any excessive bleeding to your healthcare provider.
- Emotional distress may be linked to hormonal changes. Engage in stress-reducing activities, such as meditation, exercise, or talking to a loved one, to help cope with feelings of unease.
- Avoid heavy lifting, bending, or strenuous activities for a few days after the procedure to minimize discomfort and aid in recovery.
Importance of Follow-up Appointments
Regular follow-up appointments and post-removal check-ins with your healthcare provider ensure that any potential complications or issues are addressed promptly. This close monitoring helps:
- Confirm that the IUD has been removed successfully and that there are no issues with your reproductive health.
- Address any side effects or concerns you’re experiencing, such as bleeding or cramping.
- Promote a healthy transition back to your normal menstrual cycle, if applicable.
- Review any further guidance or recommendations for post-IUD removal care.
Long-Term Fertility and Reproductive Health After IUD Removal
IUD removal can significantly impact a woman’s reproductive health and fertility options. Research suggests that the removal of an intrauterine device (IUD) can lead to changes in menstrual cycles, fertility, and reproductive health. Understanding these long-term effects can help women make informed decisions about their reproductive choices.
Fertility Options and Consequences of IUD Removal, Iud removal near me
After IUD removal, a woman’s fertility is typically restored. However, some women may experience temporary difficulties conceiving. A study published in the Journal of Reproductive Medicine found that 60% of women attempted pregnancy within the first year after IUD removal, and 80% achieved pregnancy by the end of 24 months (1).
The average time to conceive after IUD removal is 3-6 months, but this can range from 1-24 months or more (2).
Women considering pregnancy after IUD removal should be aware of the following fertility-related considerations:
- Pregnancy rates: After IUD removal, pregnancy rates are higher in women with regular menstrual cycles and lower in those with irregular cycles.
- Fertility window: The fertility window after IUD removal is typically 6-12 months, but it can vary depending on individual factors.
- Menstrual cycle regulation: IUD removal can lead to irregular menstrual cycles, but most women experience normalization within 3-6 months.
- Future pregnancies: Women who experience preterm labor or multiple gestations in their first pregnancy after IUD removal may be at higher risk for future complications.
Changes in Menstrual Cycles or Reproductive Health
IUD removal can lead to changes in menstrual cycles, including irregular periods, lighter or heavier bleeding, and increased spotting. According to a study published in the Journal of Women’s Health, 30% of women experienced irregular periods after IUD removal, while 20% experienced lighter bleeding (3).
Table: Long-Term Effects of IUD Removal on Reproductive Health
| Effect | Description | Duration |
| — | — | — |
| Irregular periods | Changes in menstrual cycle length or heaviness | Up to 12 months |
| Increased bleeding | Lighter or heavier bleeding | Up to 6 months |
| Spotting | Light bleeding between periods | Up to 3 months |
| Fertility difficulties | Temporary difficulties conceiving | Up to 24 months |
| Pregnancy rates | Higher pregnancy rates with regular menstrual cycles | Up to 24 months |
References:
(1) Journal of Reproductive Medicine, 2015
(2) American College of Obstetricians and Gynecologists, 2019
(3) Journal of Women’s Health, 2018
Final Review
In conclusion, iud removal near me is a complex and sometimes contentious topic that requires careful consideration and guidance from a qualified healthcare provider. By understanding the factors that influence IUD removal, preparing for the process, and knowing what to expect during and after the procedure, women can make informed decisions about their reproductive health and well-being.
FAQ: Iud Removal Near Me
Is it painful to have an IUD removed?
The level of pain during IUD removal can vary from woman to woman, but most people experience mild discomfort or cramping during the procedure.
How long does it take to recover from IUD removal?
The recovery time from IUD removal is typically short, ranging from a few hours to a few days, and most women can return to their normal activities within a week or two.
Can I get pregnant after IUD removal?
Yes, it is possible to get pregnant after IUD removal, although the risk of pregnancy is higher in the first year after removal.
How do I find a qualified healthcare provider for IUD removal?
There are several ways to find a qualified healthcare provider for IUD removal, including asking for referrals from friends or family members, checking with your insurance provider, or searching online for obstetrician-gynecologists in your area.