Kicking off with frenectomy near me, it’s a vital procedure to remove or shorten frenum tissue, which can be a game-changer for people dealing with various oral conditions. From treating tongue-tie in newborns to addressing issues like frenulum of the upper lip and frenulum of the lower lip, a skilled oral surgeon can provide excellent results. In this guide, we’ll walk you through the ins and outs of frenectomy near me, covering the common reasons for the procedure, how to prepare, what to expect during the surgery, and post-operative care.
So, what makes a frenectomy near me so essential? The answer lies in understanding the importance of frenum anatomy in our overall oral health. A frenum is a band of tissue that connects the tongue or lip to the jawbone. If it becomes too tight, a frenectomy might be necessary to restore comfort and function. Our top oral surgeons will guide you through each step, explaining how they approach every patient’s unique case.
Common medical conditions that necessitate a frenectomy near me
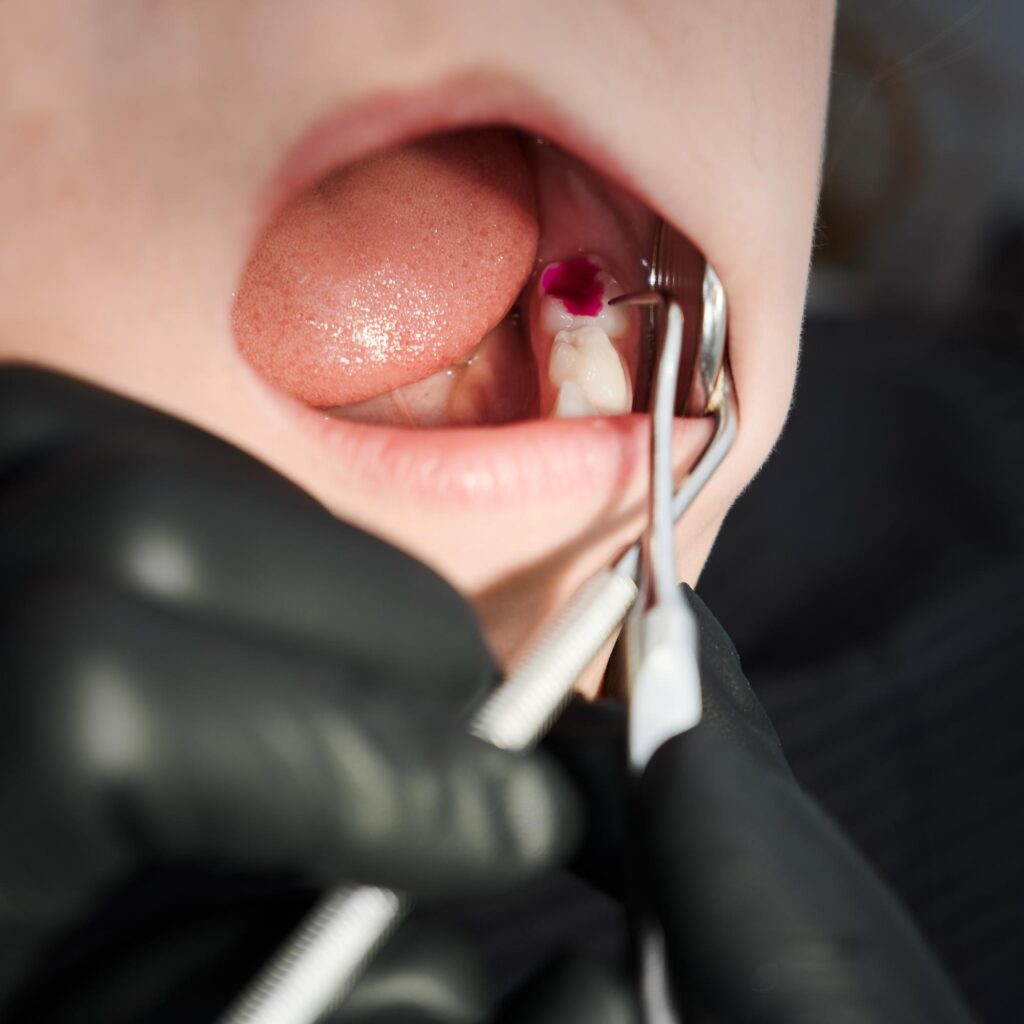
In many cases, individuals experience difficulties related to the frenulum, a small band of tissue that connects the tongue or lips to the gums and the bottom of the mouth. This condition often necessitates surgical intervention in the form of a frenectomy to improve oral health and alleviate related symptoms.
A frenectomy is a procedure that involves surgically removing the frenulum, and it can be an effective solution for addressing issues associated with the frenulum. Various medical conditions necessitate this type of surgery, often related to the tongue and the associated anatomy.
Tongue-Tied (Ankyloglossia)
Tongue-tied individuals often experience difficulties when trying to move the tongue freely in the mouth. This condition can lead to difficulties with speech, eating, and other functions, affecting overall quality of life. In severe cases, the restriction posed by an overly tight frenulum can cause breathing difficulties, as the ability to extend the tongue can become impaired.
- Restricted tongue movement leads to difficulty articulating speech sounds, especially at the back of the mouth.
- Increased stress on the palate and gums due to prolonged effort to move the tongue.
Upper Lip Tie (Frenulum of the Upper Lip)
An upper lip frenulum may also necessitate surgical removal to address associated symptoms. In individuals with an enlarged frenulum, issues related to breastfeeding may arise, affecting both babies and mothers. Furthermore, issues such as misaligned teeth or difficulties during mouth movements can also appear.
- Difficulty with breastfeeding: A long or overly tight upper lip frenulum may prevent effective latching during breastfeeding.
- Oral health complications: Overcrowded or misaligned teeth may arise when the restricted upper lip movement prevents proper oral hygiene.
Lower Lip Tie (Frenulum of the Lower Lip)
Individuals may experience difficulties related to the lower lip frenulum, which often leads to dental issues, difficulties with dental hygiene, and aesthetic problems. In such cases, a frenectomy is performed to alleviate these symptoms and to maintain optimal oral health.
- Orthodontic issues: Misaligned teeth may result due to restricted lower lip movement.
- Difficulty with tongue movement: The frenulum of the lower lip can also restrict tongue movement, leading to breathing and speech problems.
Comparing the Anatomy with the Overall Oral Anatomy
The Frenulum, whether it is the upper lip frenulum, the lower lip frenulum or even the tongue frenulum, are small, usually insignificant, parts of the oral anatomy. The entire oral cavity is made up of many different structures, including the lips, tongue, palate, gums, and teeth.
The frenulum attaches to the bottom of the mouth where it is attached to these structures. The anatomy of the oral cavity involves a complex set of relationships between the aforementioned structures and the frenulum.
- The gums support the teeth, while also acting as a protective barrier against infections and decay.
- The palate, located in the roof of the mouth, provides vital support for the upper teeth, which helps maintain proper alignment and chewing function.
Oral Surgeons’ Approach to Each Patient’s Frenectomy Procedure
Oral surgeons have varying approaches to each patient’s frenectomy procedure, as each individual’s anatomy presents unique challenges and potential complications. While addressing the specific frenulum, consideration is made for the entire oral anatomy involved in the procedure.
The overall goal remains the same: to ensure the optimal removal of the frenulum, thereby promoting overall oral health. Depending on the patient’s health status and specific anatomy, surgeons may employ a variety of techniques to address complications during or after the procedure.
The oral surgeon may consider various aspects to optimize results, including patient history, the location and extent of the frenulum, and associated underlying conditions.
- The patient’s medical history may indicate certain risks or complications associated with the procedure.
- The exact location and extent of the frenulum will determine the approach and necessary steps to achieve optimal results.
- The surgeon’s expertise in addressing specific types of frenectomy, as well as their experience with addressing associated complications, will also influence the surgical approach.
How to prepare for a frenectomy near me
Preparing for a frenectomy is a crucial step in ensuring a smooth and successful procedure. Before the surgery, it’s essential to prepare physically and mentally to minimize any discomfort or complications. Your provider will guide you through the preparation process, but here are some general steps to follow.
Pre-Operative Preparations
- Stop smoking and nicotine products: Smoking and nicotine can slow down the healing process, so it’s recommended to quit at least two weeks before the surgery. This will improve circulation and reduce the risk of complications.
- Avoid blood-thinning medications: Certain medications like aspirin, warfarin, and heparin can increase the risk of bleeding during and after the surgery. Your provider will advise you on which medications to stop taking and when to resume them.
- Get a complete medical history: Your provider will need a complete medical history, including any previous surgeries, medical conditions, and allergies. This information will help them develop a personalized treatment plan.
- Follow a healthy diet: A healthy diet rich in fruits, vegetables, and whole grains can help your body heal faster. Avoid sugary and processed foods that can slow down the healing process.
- Get enough rest: Get plenty of rest before the surgery to ensure you’re well-rested and recovered. Lack of sleep can increase stress levels, which can negatively impact the healing process.
Surgery Day Preparations
| Preparation | Surgery Day | Recovery | Follow-up |
|---|---|---|---|
| Stop medications and smoking | Arrive at the clinic on time | Follow post-operative instructions | Attend follow-up appointments |
| Get a complete medical history | Remove jewelry and valuables | Take pain medication as prescribed | Report any complications or concerns |
| Fill out consent forms | Bring a companion for support | Avoid strenuous activities | Follow up with the provider |
Importance of Post-Operative Care
Post-operative care is crucial for optimal healing and minimize complications. Follow your provider’s instructions carefully, and don’t hesitate to reach out if you have any questions or concerns. Here are some essential steps to take during the recovery period:
- Follow pain management plan: Take pain medication as prescribed by your provider to manage discomfort and pain.
- Avoid strenuous activities: Avoid bending, lifting, or strenuous activities that can disrupt the healing process.
- Keep the area clean: Keep the wound area clean and dry to prevent infection.
- Follow dietary instructions: Follow a balanced diet that promotes healing and minimizes inflammation.
Importance of Follow-up Appointments
Follow-up appointments are essential to ensure the healing process is progressing as expected. Attend all scheduled appointments, and don’t hesitate to reach out if you have any questions or concerns. Your provider will assess your progress, address any complications, and provide guidance on how to maintain optimal oral health.
What to expect during a frenectomy near me
A frenectomy is a relatively straightforward procedure that involves the removal or repositioning of a frenum, which is a small band of tissue that can restrict movement or cause discomfort. During a frenectomy, your surgeon will work to carefully remove or reposition the frenum, taking care to minimize any discomfort or potential complications.
The Surgical Process
The surgical process for a frenectomy typically involves the following steps:
The surgeon will begin by administering local anesthesia to numb the area where the frenectomy will be performed. This will help to minimize any discomfort or pain during the procedure. Once the anesthesia has taken effect, the surgeon will use a specialized tool to carefully remove or reposition the frenum.
The frenum will be carefully dissected and removed, taking care to preserve any surrounding tissue. In some cases, the surgeon may use a laser or other specialized tool to aid in the removal of the frenum.
Once the frenum has been removed or repositioned, the surgeon will close the incision site with sutures or staples. In some cases, the surgeon may use a topical antibiotic ointment to promote healing and prevent infection.
Use of Local Anesthesia and Sedation
Local anesthesia and sedation are commonly used during a frenectomy to help minimize discomfort or anxiety. Local anesthesia numbs the area where the frenectomy will be performed, while sedation can help to promote relaxation and reduce any anxiety or stress.
The type and dosage of local anesthesia and sedation used will depend on the individual patient and the specific needs of the procedure. In some cases, the patient may be given a light sedative to help promote relaxation, while in other cases, the patient may be given a more potent anesthetic to ensure comfort during the procedure.
The surgeon will closely monitor the patient’s vital signs and responses during the procedure, making adjustments to the anesthesia and sedation as needed to ensure the patient’s comfort and safety. Patients are generally able to go about their daily activities within a few days of the procedure, with minimal discomfort or pain.
Potential Complications and Risks
While a frenectomy is generally a safe and straightforward procedure, there are some potential complications and risks to be aware of. These may include:
– Bleeding or discharge: In some cases, patients may experience bleeding or discharge at the incision site during the healing process. This is typically not a cause for concern and can be easily treated with antibiotic ointment and dressings.
– Infection: As with any surgical procedure, there is a risk of infection with a frenectomy. Patients are usually given antibiotics to reduce this risk and promote healing.
– Scarring: In some cases, patients may be left with noticeable scarring at the incision site. This can often be minimized with proper wound care and follow-up appointments with the surgeon.
– Nerve damage: There is a small risk of nerve damage during the procedure, which can result in numbness, tingling, or weakness in the affected area. This is typically temporary but may in some cases be permanent.
– Frenulum recession: In some cases, the frenulum may experience recession or retraction after the procedure. This can be treated with additional surgery or observation.
Questions to Ask Your Surgeon
When meeting with your surgeon to discuss a frenectomy, it’s essential to ask the right questions to ensure you have a clear understanding of the procedure and what to expect. Here are some questions to consider:
– What are the potential complications and risks associated with a frenectomy?
– How will the procedure be performed, and what type of anesthesia will be used?
– How long will the procedure take, and what is the expected recovery time?
– What are the chances of successful outcome, and what are the potential outcomes if the procedure is not successful?
– Are there any specific preoperative or postoperative instructions I should follow?
– How will I know if the procedure has been successful, and what follow-up appointments will I need to schedule?
– Are there any additional procedures or treatments that may be needed to achieve the desired results?
Post-operative care for a frenectomy near me
A successful frenectomy outcome largely depends on the patient’s ability to recover effectively after the procedure. Many patients who have undergone a frenectomy with proper care have experienced a smooth and uneventful recovery. For instance, a patient who underwent a frenectomy to address a tongue-tie issue reported feeling relief from discomfort and improved feeding experience for their baby, with no noticeable complications during the recovery period.
In our experience, patients who have diligently followed their doctor’s post-operative care instructions have experienced fewer complications and a faster recovery. This highlights the importance of proper post-operative care, which we will discuss in this section.
Role of antibiotics in preventing post-surgical infections
Antibiotics play a significant role in preventing post-surgical infections, including those that may occur after a frenectomy. According to the American Dental Association (ADA), the use of antibiotics in dental procedures is a common practice to prevent infection. This is especially important in procedures like frenectomy, which involve incision and suturing of soft tissues.
During the recovery period, antibiotics may be prescribed to prevent infection. It is essential for patients to complete the entire course of antibiotics as directed by their doctor to ensure that any potential infection is fully eradicated.
Here are some examples of antibiotics that may be prescribed after a frenectomy:
- Amoxicillin
- Cephalexin
- Clindamycin
These antibiotics work by targeting specific types of bacteria that may cause infection. It is crucial for patients to follow their doctor’s instructions carefully and complete the full course of antibiotics, even if symptoms appear to be resolving.
Avoiding certain foods and activities during recovery
After a frenectomy, it is essential to avoid certain foods and activities that may interfere with the healing process or increase the risk of complications. Here are some examples of foods and activities to avoid during the recovery period:
- Foods that are difficult to chew or swallow, such as nuts, seeds, or hard candies
- Spicy or acidic foods that may irritate the wound
- Sleeping on the side or stomach, as this may put pressure on the wound
- Smoking or using smokeless tobacco, as these substances can impair healing
It is also essential to follow a soft food diet during the recovery period. This may include foods like yogurt, scrambled eggs, mashed bananas, or applesauce.
Comparing and contrasting different post-operative pain management options, Frenectomy near me
There are several post-operative pain management options available after a frenectomy, each with its benefits and drawbacks. Here are some common options:
- Over-the-counter pain medications like ibuprofen or acetaminophen
- Prescription pain medications like oxycodone or hydrocodone
- Nerve blocks or local anesthetic injections
- Ice packs or cold compresses
It is essential to discuss the best pain management option with your doctor, as they can provide personalized guidance based on your individual needs and medical history. Some patients may respond better to one type of pain management than another, so it is crucial to explore different options until finding the most effective solution.
Final Conclusion

In conclusion, frenectomy near me is a straightforward yet effective procedure that requires careful preparation and a skilled surgeon. Whether you’re dealing with a tongue-tie or another form of oral restriction, our comprehensive guide will empower you to take the first step towards restoring your oral health. Consult with an experienced oral surgeon in your area to learn more about your options and to find the perfect fit for your needs.
Answers to Common Questions
How long does a frenectomy take?
Typically, a frenectomy near me procedure takes anywhere from 30 minutes to an hour, depending on the complexity of the case and whether the patient is under sedation or local anesthesia.
Is a frenectomy painful?
No, frenectomies are relatively painless due to the use of local anesthesia. Patients might feel some minor discomfort afterward, but this can be managed with pain medication as prescribed by the surgeon.
Can a frenectomy be done on an infant?
Yes, frenectomies can be performed on infants, usually within the first few months of life. The procedure is usually done under general anesthesia, and the goal is to release the tongue or lip frenum to facilitate proper growth and development.
How long does it take to recover from a frenectomy?
The recovery period for a frenectomy near me typically lasts a few days, during which time patients may experience soreness, swelling, and temporary difficulty eating or drinking. However, most patients can return to their normal routine within a week or two.