Pediatric Otolaryngology Near Me takes center stage, bringing good knowledge into a world crafted with absorbing reading experience. When searching for a pediatric otolaryngologist, it is essential to consider the unique aspects of pediatric otolaryngology, the necessary skills and qualifications for the specialist, and the specialties and sub-specialties of pediatric otolaryngology.
This opening passage provides a glimpse into the essential qualities and qualifications of a pediatric otolaryngologist, including their ability to work with young patients, understand the developing anatomy and physiology of children’s ears, nose, and throat, and collaborate with other healthcare professionals. With advanced technologies and techniques, including 3D printing and ultrasound imaging, pediatric otolaryngologists can provide more effective patient care.
Unique Aspects of Pediatric Otolaryngology That Distinguish It From Other Medical Fields
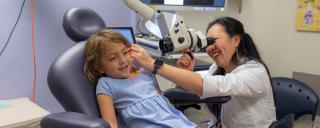
Pediatric otolaryngology, often referred to as pediatric ENT or pediatric ear, nose, and throat care, is a specialized medical field that deals with the diagnosis and treatment of ear, nose, and throat disorders in infants, children, and adolescents. This unique branch of medicine requires a deep understanding of the developing anatomy and physiology of children’s ears, nose, and throat, as well as the distinct challenges and opportunities presented by pediatric patients.
Dynamic Anatomy and Physiology, Pediatric otolaryngology near me
The developing anatomy and physiology of children’s ears, nose, and throat create unique considerations for diagnosis and treatment. Children’s ears, for example, are still developing and are more prone to infection and damage. The Eustachian tube, which helps regulate air pressure in the ear, is not fully developed until around age 5. This can lead to difficulties in treating ear infections and preventing hearing loss in young children.
Children’s nasal passages and sinuses are also still developing and are more prone to congestion and respiratory infections. The adenoids, which are lymphoid tissues located in the back of the throat, are larger and more active in children, making them more prone to infections and tonsillitis. As a result, pediatric otolaryngologists must be aware of these anatomical and physiological differences when diagnosing and treating ear, nose, and throat disorders in children.
Developmental Considerations
Understanding the developing anatomy and physiology of children’s ears, nose, and throat is crucial for effective diagnosis and treatment. In children under the age of 2, for example, ear infections can be more challenging to diagnose and treat due to their small ear canals and sensitive eardrums. In older children, tonsillitis and adenoiditis require careful consideration of the child’s developmental stage and the potential impact of treatment on their quality of life.
Challenges of Pediatric Diagnosis
Diagnosing ear, nose, and throat disorders in children can be a challenging task due to their inability to verbalize their symptoms and the difficulty of performing invasive procedures. Pediatric otolaryngologists must be skilled in using various diagnostic tools, such as audiology testing and imaging studies, to accurately diagnose and treat ear, nose, and throat disorders in children.
Examples of Effective Patient Care
Understanding the unique aspects of pediatric otolaryngology can lead to more effective patient care in the following situations:
*
Ear Infections in Young Children
A 6-month-old infant presents with a fever and ear pain. The pediatric otolaryngologist recognizes the infant’s small ear canals and sensitive eardrums, and carefully diagnoses and treats the ear infection with antibiotic therapy. The patient’s symptoms improve, and they are able to hear and communicate more effectively.
*
Tonsillitis in School-Age Children
A 9-year-old child presents with recurrent tonsillitis and sleep disturbances. The pediatric otolaryngologist considers the child’s developmental stage and the potential impact of treatment on their quality of life, and decides to perform a tonsillectomy to alleviate the symptoms and improve the child’s sleep. The patient’s symptoms improve, and they are able to sleep and concentrate more effectively.
*
Adenoiditis in Toddlers
A 2-year-old child presents with recurrent adenoiditis and respiratory infections. The pediatric otolaryngologist recognizes the child’s larger and more active adenoids, and recommends adenoidectomy to alleviate the symptoms and reduce the risk of recurrent infections. The patient’s symptoms improve, and they are able to breathe and sleep more effectively.
*
Speech and Language Development in Children
A 3-year-old child presents with speech and language difficulties due to a hearing impairment. The pediatric otolaryngologist recognizes the child’s developing anatomy and physiology, and recommends amplification therapy to improve the child’s hearing and facilitate speech and language development. The patient’s symptoms improve, and they are able to communicate more effectively with their caregivers and peers.
Essential Skills and Qualifications for Pediatric Otolaryngologists
Pediatric otolaryngologists require a unique blend of medical knowledge, communication skills, and emotional resilience to provide comprehensive care to children with ear, nose, and throat conditions. Developing a strong foundation in medical education and pursuing ongoing professional development are crucial to remain current with the latest techniques and advancements in the field.
Key Qualities for Pediatric Otolaryngologists
To be successful, pediatric otolaryngologists should possess the following essential qualities and characteristics.
- Compassionate Communication
Pediatric otolaryngologists must be able to communicate effectively with children, parents, and other healthcare professionals. Developing a patient-centered approach and using clear, simple language when explaining medical information helps alleviate anxiety and ensures informed decision-making. - Emotional Resilience
Working with children who may face chronic illness, disability, or trauma requires exceptional emotional resilience. Pediatric otolaryngologists must be able to manage stress, maintain a positive attitude, and prioritize self-care to provide high-quality care. - Clinical Expertise
Pediatric otolaryngologists must possess in-depth knowledge of pediatric ear, nose, and throat conditions, as well as stay up-to-date with the latest research and treatment options. This requires ongoing education and participation in professional societies to advance their skills and expertise. - Collaboration and Teamwork
Pediatric otolaryngologists often work within multidisciplinary teams, requiring strong collaboration and communication skills to coordinate care with other specialists, including otologists, audiologists, and allergists. - Adaptability and Flexibility
Pediatric otolaryngologists must be able to adapt to changing medical information, new technologies, and evolving patient needs, demonstrating flexibility and a willingness to learn and grow.
Ongoing Education and Professional Development
To stay current with the latest advancements and innovations in pediatric otolaryngology, professionals in this field should engage in ongoing education and professional development. This can include:
- Attending conferences and workshops
Regular participation in conferences and workshops provides opportunities to learn from leading experts and network with peers. - Online courses and webinars
Online learning platforms offer flexible, self-paced learning opportunities to enhance knowledge and skills. - Professional society membership
Joining professional societies, such as the American Academy of Otolaryngology-Head and Neck Surgery, provides access to expert resources, research, and educational opportunities.
Collaboration with Other Healthcare Professionals
Effective collaboration with other healthcare professionals is essential in pediatric otolaryngology. Two examples of effective partnerships are:
- Multidisciplinary care teams
Collaborative care teams involving pediatric otolaryngologists, otologists, audiologists, and allergists work together to provide comprehensive care for children with complex ear, nose, and throat conditions. - Primary care physician partnerships
Pediatric otolaryngologists often work closely with primary care physicians to provide early screening, diagnosis, and referral for children with ear, nose, and throat concerns.
Effective Partnerships in Pediatric Otolaryngology
Effective partnerships in pediatric otolaryngology involve ongoing communication, mutual respect, and a shared commitment to delivering high-quality care. Examples of successful collaborations include:
- Regular communication and consultation
Regular communication and consultation between pediatric otolaryngologists and other healthcare professionals ensures seamless care coordination and promotes a unified approach to patient care. - Shared decision-making
Shared decision-making with patients, families, and other healthcare professionals promotes patient-centered care, ensures informed decision-making, and fosters a sense of collaboration and cooperation.
Finding the Right Pediatric Otolaryngologist Near You: Pediatric Otolaryngology Near Me
With the complexities involved in pediatric care, finding a qualified and experienced pediatric otolaryngologist is crucial for the optimal treatment and care of your child’s ear, nose, and throat ailments. A dedicated pediatric otolaryngologist will be well-equipped to address the unique needs and concerns of parents or guardians who are seeking the best possible care for their child.
Qualities and Qualifications to Look for in a Pediatric Otolaryngologist
When searching for a pediatric otolaryngologist near you, it’s essential to consider the following essential qualities and qualifications. A pediatric otolaryngologist should possess a deep understanding of the unique needs of children and adolescents, and be able to communicate effectively with patients and families.
| Qualification | Description |
|---|---|
| Board Certification | A pediatric otolaryngologist who is board certified by the American Board of Otolaryngology or the American Osteopathic Board of Otolaryngology has undergone rigorous training and assessment to demonstrate their expertise and commitment to providing high-quality care. |
| Experience in Pediatric Care | A pediatric otolaryngologist with significant experience in caring for children and adolescents will be better equipped to address the unique needs and concerns of young patients and their families. |
| Communication Skills | A pediatric otolaryngologist who can effectively communicate with patients and families is essential for building trust and ensuring that the child’s needs are met. |
| Continuity of Care | A pediatric otolaryngologist who provides comprehensive care and coordinates with other healthcare professionals to ensure continuity of care will be essential in managing complex ear, nose, and throat conditions. |
Effective Communication with a Pediatric Otolaryngologist
Open and honest communication is crucial when working with a pediatric otolaryngologist. Patients and families should feel comfortable asking questions, sharing their concerns, and discussing their child’s condition in a safe and non-judgmental environment.
- Be honest and open about your child’s medical history and any concerns you may have.
- Ask questions and seek clarification if you’re unsure about any aspect of your child’s care.
- Discuss your family’s values and preferences regarding your child’s care to ensure that you’re on the same page as the pediatric otolaryngologist.
- Foster a relationship with the pediatric otolaryngologist and their staff to build trust and ensure that your child receives comprehensive care.
Building Trust and Rapport with Young Patients and Families
A pediatric otolaryngologist who can build trust and rapport with their young patients and families will be better equipped to provide high-quality care and manage complex ear, nose, and throat conditions.
- Take the time to understand the child’s needs and concerns, and communicate effectively with them and their family.
- Provide personalized care planning and education to help families make informed decisions about their child’s care.
- Use age-appropriate language and explanations to ensure that children and adolescents understand their condition and treatment plan.
- Foster a positive and supportive relationship with families to help build trust and ensure continuity of care.
Current Technologies and Techniques in Pediatric Otolaryngology
The field of pediatric otolaryngology has witnessed remarkable advancements in recent years, driven by innovative technologies and techniques. These advancements have revolutionized the diagnosis, treatment, and management of complex ear, nose, and throat conditions in children. In this section, we will explore the current technologies and techniques that are transforming the landscape of pediatric otolaryngology.
Advanced Imaging Techniques
Advanced imaging techniques have played a vital role in pediatric otolaryngology, allowing for precise diagnosis and monitoring of ear, nose, and throat conditions in children. Two notable examples are 3D printing and ultrasound imaging.
- 3D Printing: 3D printing technology enables the creation of detailed, custom-designed models of the ear, nose, and throat anatomy. These models can be used for surgical planning, rehearsal, and education. For instance, otolaryngologists can create 3D models of a child’s ear to plan and practice a complex surgery, such as a labyrinthectomy. This minimizes the risk of complications and improves surgical outcomes.
- Ultrasound Imaging: Ultrasound imaging is a non-invasive, painless, and cost-effective diagnostic tool that uses high-frequency sound waves to create detailed images of the ear, nose, and throat. It is particularly useful for assessing the integrity of the tympanic membrane, the presence of middle ear effusion, and the patency of the Eustachian tube.
Innovative Surgical Techniques
Pediatric otolaryngologists employ various innovative surgical techniques to address complex ear, nose, and throat conditions in children. Two notable examples are endoscopic ear surgery and robotic-assisted surgery.
- Endoscopic Ear Surgery: Endoscopic ear surgery involves the use of flexible or rigid endoscopes to visualize the ear canal and middle ear structures. This technique allows for minimally invasive surgery, reducing the need for external incisions and minimizing the risk of complications. Endoscopic ear surgery is particularly useful for treating conditions such as chronic otitis media, ear drums perforation, and ossicular chain defects.
- Robotic-Assisted Surgery: Robotic-assisted surgery uses a robotic system to enhance the precision and dexterity of surgical procedures. In pediatric otolaryngology, robotic-assisted surgery is utilized for complex operations such as adenoidectomy, tonsillectomy, and laryngotracheal reconstruction. The robotic system enables surgeons to perform delicate dissections, improve visualization, and reduce post-operative complications.
Communication and Telemedicine
The advent of technology has transformed the way pediatric otolaryngologists communicate with patients and families. Telemedicine and online portals have enabled remote consultations, improving access to care, reducing waiting times, and enhancing patient engagement.
- Telemedicine: Telemedicine platforms enable secure, real-time communication between patients, families, and healthcare providers. Regular virtual check-ins can facilitate timely assessments, treatment plans, and follow-up care, ensuring seamless continuity of care.
- Online Portals: Patient engagement platforms and online portals allow patients and families to access medical records, communicate with healthcare providers, and participate in care decision-making. These tools facilitate informed decision-making, improved health literacy, and enhanced patient satisfaction.
Wrap-Up
In conclusion, finding the right pediatric otolaryngologist near you requires a combination of knowledge about the field, the necessary skills and qualifications, and the ability to communicate effectively with young patients and families. By choosing a pediatric otolaryngologist who possesses the qualities and qualifications mentioned above, individuals can receive the best possible care for their ear, nose, and throat conditions.
FAQ Guide
Q: What are the unique aspects of pediatric otolaryngology?
Pediatric otolaryngology is a unique field that requires specialists to understand the developing anatomy and physiology of children’s ears, nose, and throat, and to work with young patients who may not be able to communicate their needs effectively.
Q: What skills and qualifications do pediatric otolaryngologists need to possess?
Pediatric otolaryngologists need to possess excellent communication skills, the ability to work with young patients and families, and knowledge of the latest techniques and innovations in the field.
Q: What are the specialties and sub-specialties of pediatric otolaryngology?
Some specialties and sub-specialties of pediatric otolaryngology include ear infections, voice disorders, and airway management, among others.
Q: How do pediatric otolaryngologists use advanced technologies and techniques in their practice?
Pediatric otolaryngologists use advanced technologies and techniques such as 3D printing and ultrasound imaging to provide more effective patient care.